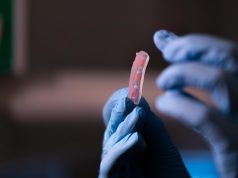
A Research team at Northwestern University has developed a 3D printable material to create custom bone implants of any shape and size, promoting bone regeneration and growth.
Over the past few years a lot of research has been done in regards to finding a suitable materiale for bone reconstruction. Now engineers at Northwestern University have made a possible breakthrough by developing a 3D printable biomaterial they call “hyperelastic bone”. Since the material induces bone growths, it could be especially useful for the treatment of bone loss in children. As children are still growing, metallic and other implants are often not an option as they need to be replaced as their body is growing. Often surgeons get the missing bone from elsewhere in the body, leading to other complications.
3D bioprinting opens up a completely new world of options for doctors, as they would ideally be able to create 3D printable, customised bone implants that will eventually become a part of the patients body due to the cells growing on it.
Ramille N. Shah, assistant professor of materials science and engineering at Northwestern’s McCormick School of Engineering and her team have developed a 3D printable biomaterial that is a mixture of a calcium mineral found naturally in human bone, called hydroxyapatite, and a biocompatible, biodegradable polymer used in medical applications. However, important is the 3D printed porous structure, that allows for new cells and blood vessels to form, as Shah explains: “Porosity is huge when it comes to tissue regeneration, because you want cells and blood vessels to infiltrate the scaffold. Our 3-D structure has different levels of porosity that is advantageous for its physical and biological properties.”
So far trials in in-vivo animal models have shown promising results.
Although hydroxyapatite is a great material to promote bone regeneration, it is also a very tricky material to work with. Being hard and brittle, researchers usually compensate for that by using a high amount of polymers. This, on the other hand, prevents the calcium biomaterial from being active on the scaffold. Shah and her team were able to achieve a weight ratio of 90% to 10% for hydroxyapatite to polymer. It still maintains its elasticity due to the design of the printed structure.
“Cells can sense the hydroxyapatite and respond to its bioactivity,” Shah explained. “When you put stem cells on our scaffolds, they turn into bone cells and start to up-regulate their expression of bone specific genes. This is in the absence of any other osteo-inducing substances. It’s just the interaction between the cells and the material itself.”
Additionally, the researchers were also able to incorporate other substances such as antibiotics into the bio-ink to produce the scaffolds: “We can incorporate antibiotics to reduce the possibility of infection after surgery. We also can combine the ink with different types of growth factors, if needed, to further enhance regeneration. It’s really a multi-functional material.”
Shah expects a bright future for patients in need of implants, with 3D printers being accessible at hospitals: “The turnaround time for an implant that’s specialized for a customer could be within 24 hours.That could change the world of craniofacial and orthopaedic surgery, and, I hope, will improve patient outcomes.”
Link to study: Hyperelastic “bone”: A highly versatile, growth factor–free, osteoregenerative, scalable, and surgically friendly biomaterial
Subscribe to our Newsletter
3DPResso is a weekly newsletter that links to the most exciting global stories from the 3D printing and additive manufacturing industry.