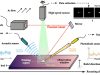
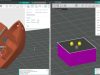
Specialists from the University Hospital of Toulouse and the Claudius Regaud Institute have performed a nose reconstruction on a patient at the Cancer Institute of the University of Toulouse-Oncopole. For this complete reconstruction, the doctors used new technologies such as 3D printing.
The patient had been treated in 2013 for nasal cavity cancer (squamous cell carcinoma) with radiotherapy and chemotherapy. As a result of this treatment, she lost a large part of her nose as well as the front part of her palate. For more than four years, she lived without a nose, faced with failed nasal reconstruction skin flap grafting and difficulty in wearing a facial prosthesis. She was offered a custom–made biomaterial nasal reconstruction, based on a two–stage surgical procedure performed by Pr. Agnès Dupret Bories and Dr. Benjamin Vairel.
This type of reconstruction had never been performed on such a fragile and poorly vascularized area and was made possible thanks to the collaboration of the medical teams with Cerhum, a Belgian medical device manufacturer specializing in bone reconstruction. This new technique also makes it possible to overcome certain limitations presented by other techniques. The collaboration of these two entities took place through the PhD thesis carried out by a PhD student of Cerhum and the CIRIMAT laboratory (Inter– university center of research and engineering of materials/CNRS/University Toulouse III–Paul–Sabatier).
Successful transplantation
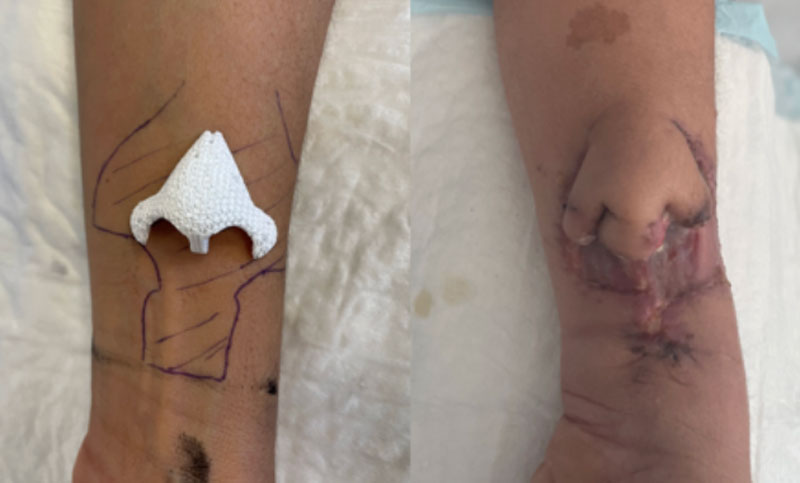
The biomaterial used to reconstruct the patient’s nose was 3D printed after several discussions between Cerhum’s engineers and the surgical team based on 3D views taken before the cancer treatment was started. The biomaterial was first placed under the skin (implanted) for vascularization on the patient’s forearm.
Biomaterials are materials, synthetic or living, that can be used for medical purposes to replace a part or function of an organ or tissue.
In September 2022, two months after implanting the bone graft under the patient’s skin, the colonisation of the medical device was complete. The device device was transplanted to the nasal area and successfully revascularised using microsurgery by anastomosing (creating a connection between blood vessels) the vessels of the skin of the arm to vessels in the patient’s temple.
After ten days in hospital and three weeks of antibiotics, the patient is doing very well.
Find out more about the University Hospital of Toulouse at iuct-oncopole.fr.
Subscribe to our Newsletter
3DPResso is a weekly newsletter that links to the most exciting global stories from the 3D printing and additive manufacturing industry.